POEM (Per Oral Endoscopic Myotomy)
Achalasia
The Treatment
POEM (Per Oral Endoscopic Myotomy)
Surgery and POEM
Laparoscopic (keyhole surgery) division of the lower oesophageal sphincter (Heller myotomy) has been the first line treatment for Achalasia. Myotomy is a surgical procedure in which the lower oesophageal sphincter muscle is cut to allow the oesophagus to open. Heller myotomy is the most common technique used. This is usually followed by fundoplication, where part of the stomach is wrapped around the oesophagus to avoid the backflow of the stomach's contents following the surgery. The surgery allows food to pass easily into the stomach.
The latest technique that is now available as an alternative technique for myotomy is called Per Oral Endoscopic Myotomy or POEM. POEM was first performed in Australia by Assoc. Prof. Crosthwaite. This technique involves doing the myotomy using a flexible telescope which is passed through the mouth down the oesophagus to perform the procedure so that no cuts are required on the abdomen.
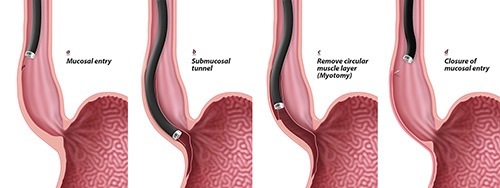
Procedure
POEM – Per Oral Endoscopic Myotomy
This is the most up to date treatment for Achalasia. This is a new treatment that Assoc. Prof. Crosthwaite has introduced in Australia. It is undertaken using a gastroscope, which is a flexible fibreoptic telescope passed through the mouth into the oesophagus, without any cuts on the abdomen. Using a special knife the muscle is approached by tunnelling under the lining of the oesophagus. Once this is done the myotomy is done by cutting the lower oesophageal sphincter as well as the inner layers of the oesophageal muscle with this special knife. The telescope is then removed and the opening is closed with special clips. No open or keyhole incisions are required using this approach.
This procedure has been shown to be very safe and to date the outcomes have been very successful with rapid recovery and improvement in swallowing.
Currently this procedure requires a stay of 1-2 days in hospital and the recovery is similar to the laparoscopic procedure.
Laparoscopic Heller Myotomy
Heller myotomy can be performed by a minimal invasive laparoscopic approach. The procedure is performed under general anaesthesia. Your surgeon will make five small incisions for a laparoscopic approach on your upper abdomen. Your surgeon will insert tiny instruments and a laparoscope, a thin tube with a lighted device and a camera at the end to view the internal organs on a screen.
Steps involved in Heller myotomy procedure:
- Your surgeon makes a lengthwise incision along the oesophagus, from just above the lower oesophageal sphincter muscle into on to the stomach. Only the outer muscles of the oesophagus are cut, leaving the inner muscosal layer untouched. The incisions will reduce the force of the contracting muscles and relax the lower oesophageal sphincter; thereby, allowing food to pass easily.
- A fundoplication is often may be performed along with the myotomy.
- To perform the fundoplication, your surgeon wraps the upper part of your stomach around the lower oesophageal sphincter.
- Myotomy and fundoplication together will allow entry of food into the stomach and at the same time prevent the acid from refluxing back into the oesophagus.
Post-operative information
Following the procedure, you may be discharged after a day or two if you have undergone either a laparoscopic procedure or POEM.
Medications will be prescribed for pain relief. Avoid heavy lifting and driving for at least 2 to 4 weeks after surgery. Inform your doctor immediately if you experience fever, nausea or vomiting, swelling in the legs, redness and odorous drainage from the incisions.
Benefits of this approach
Most of the patients who have undergone laparoscopic myotomy or POEM have found significant decrease or a complete cure of achalasia symptoms. The most important benefit of this procedure is that you are likely to have a drastic reduction in regurgitation.
Preparation
Before the procedure, you may be instructed to be on a fluid diet for a number of days prior to the procedure and not to eat or drink anything at least six hours before the procedure in order to keep the oesophagus clear. Your surgeon will give you instructions on the medications you need to avoid.
Outcome
Surgery is found to be beneficial in most of the patients. However, as with any procedure, myotomy may involve certain risks and complications, such as infection, bleeding, perforation of the oesophagus, chest pain, pneumonia and recurrence of regurgitation symptoms and symptoms such as difficulty in swallowing.
Post-op stages of recovery and care plan
Following the procedure, you will be given specific instructions with regard to your diet. In the first few two weeks after surgery, you are advised to consume liquids and soft foods. You are instructed to eat small and regular meals, take small bites and chew food well.
You will be given an anti-acid medication for at least one month after surgery.
Down-time - lifestyle or off work duration
Shortly after surgery you can gradually resume your daily activities. You are encouraged to start walking as early as possible to reduce the risks of blood clots and improve breathing. Driving can be resumed once you stop taking pain medication. You can return to work after 1-2 weeks of surgery. However, if your work requires lifting heavy objects, you can resume these activities after 6 weeks.
Costs
Any costs involved will be discussed with you prior to your surgery.
Research
Extensive research is being done to find better treatment options for achalasia. Some of the recent studies have found that:
- Peroral Endoscopic Myotomy for the Treatment of Achalasia: A Prospective Single Center Study Am J Gastroenterol 2012; 107:411–417; doi: 10.1038/ajg.2011.388; published online 8 November 2011
- Per Oral Endoscopic Myotomy for Achalasia Thorac Surg Clin 21(2011) 519-525
- Laparoscopic myotomy followed by fundoplication is the most effective surgical treatment for short and long term relief of achalasia. 1
- Botulinum toxin injection and the drug ethanolamine oleate show comparable efficacy for the treatment of achalasia. 2
There are many treatment options for achalasia and is decided upon based on your individual condition.
![]() Per-oral endoscopic myotomy (POEM)
Per-oral endoscopic myotomy (POEM)
You will need the Adobe Reader to view and print the above documents. ![]()





