Oesophageal Achalasia
Description
Oesophageal achalasia is a condition in which the oesophagus (tube carrying food from the mouth to the stomach) is unable to move food into the stomach. The muscles at the lower end of the oesophageal sphincter fail to relax and allow food to pass into the stomach, resulting in reflux.
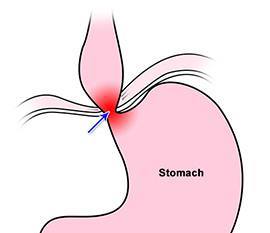
Causes
Oesophageal achalasia is caused by damage to the nerves supplying the oesophagus, which affects:
- Muscles lining the oesophagus that rhythmically contract to push food towards the stomach
- Muscles of the lower oesophageal sphincter that act as a gate for the one-way movement of food into the stomach
The cause of damage is not clear, but may be associated with an earlier viral infection or autoimmune condition, such as lupus and uveitis, but may be an immune problem where the body attacks healthy cells.
Impact
Achalasia can have a significant impact on your health with respect to the act of eating and drinking. With the advancement of the condition you may lose considerable amount of weight and suffer from malnutrition. If the obstruction lasts for a long time, there are chances of developing oesophageal cancer.
Anatomy
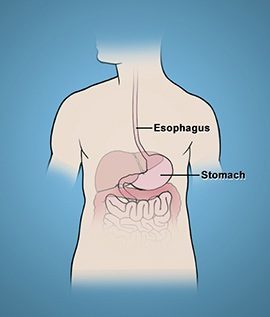
The oesophagus is a long, narrow tube that allows the passage of food from the throat to the stomach. It extends behind the windpipe and heart and in front of the spine, and passes through the diaphragm before joining the stomach. The food pipe is lined by muscles that expand and contract to push food down the tube. A valve called the upper oesophageal sphincter prevents the accidental movement of food into the windpipe. Another valve called the lower oesophageal sphincter, located at the junction of the stomach and oesophagus, allows the passage of food to the stomach and prevents the backflow of food and stomach acids into the oesophagus. The sphincter is controlled by muscles that relax and contract to open and close the passage.
Symptoms
Common symptoms of achalasia include difficulty swallowing (dysphagia) both solid and liquid foods, and experiencing the sensation of food getting stuck in the chest. To facilitate swallowing you may make changes in the way you eat. Other symptoms include regurgitation of food, heartburn, sensation of fullness and chest pain. In advanced stages of the disease, you may experience weight loss and suffer from malnutrition (although this is rare).
Diagnosis
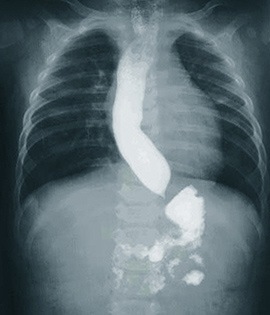
Your doctor may order the following tests to diagnose achalasia:
- Barium swallow test: involves swallowing a barium preparation, which can be detected through X-rays
- Endoscopy: allows the doctor to examine the inside of your oesophagus, stomach, and portions of the intestine, with an instrument called an endoscope, a thin flexible lighted tube
- Manometry: measures changes in pressure exerted by the oesophageal sphincter
Treatments
Treatment aims at opening or relaxing the lower oesophageal sphincter muscles for easy passage of food into the stomach. Some of the options for relieving symptoms include:
- POEM: POEM or Per Oral Endoscopic Myotomy is a new treatment being offered to allow a myotomy to be performed using a gastroscope rather than having an operation. This latest treatment is offered by Assoc. Prof. Crosthwaite
- Medications: Medications help relax the lower oesophagus sphincter muscles and provide temporary relief.
- Botox injection: Botulinum toxin injection can be administered to help relax the sphincter muscles. It provides temporary relief only and has to be repeated after a few months or years.
- Balloon dilation (pneumatic dilatation): A small balloon is positioned at the lower oesophagus sphincter and inflated to widen the opening. Although this procedure improves swallowing, it is not a permanent solution and needs to be repeated.
- Myotomy surgery: Myotomy is a surgical procedure in which the sphincter muscle is cut to open up the oesophagus. This surgery provides a permanent solution to swallowing.
Prognosis
The outcome of treatment varies from person to person. Some may experience mild symptoms while for some the treatment can be very successful. Multiple treatments may be required for others. For most patients surgery is recommended. The success rate of surgery is 70 to80 to 90%, but as with all procedures the outcome may depend on the extent of the disease
Untreated
If left untreated, achalasia may cause weight loss, malnutrition, or inflammation or ulceration of the oesophagus. The elderly may suffer from pneumonia and lung infections. Chances of developing oesophageal cancer increase for patients with untreated achalasia.





